Navigating the Discomfort of IBS
Irritable bowel syndrome (IBS) can cause significant abdominal pain, impacting daily life. This article provides eight effective strategies to answer the question, "what helps IBS pain?" Discover how a low FODMAP diet, peppermint oil, hypnotherapy, specific probiotics, stress management, soluble fiber, heat therapy, and antispasmodic medications can provide relief and improve your gut health. Learn how to manage IBS pain and reclaim a more comfortable life.
1. Low FODMAP Diet
For those seeking relief from the often debilitating pain of Irritable Bowel Syndrome (IBS), the low FODMAP diet stands out as a scientifically-backed and effective approach. If you're constantly asking yourself, "what helps IBS pain?", this dietary strategy may provide the answers you've been searching for. It focuses on eliminating and then systematically reintroducing specific types of fermentable carbohydrates (FODMAPs) that are known to trigger IBS symptoms like bloating, gas, abdominal pain, and altered bowel habits. This three-phase elimination diet helps identify specific food triggers, enabling you to create a personalized eating plan for long-term IBS management.
The low FODMAP diet isn't just another fad diet; it’s rooted in extensive clinical research and is endorsed by major institutions like the Mayo Clinic. It works by temporarily restricting FODMAPs – oligosaccharides, disaccharides, monosaccharides, and polyols – which are poorly absorbed in the small intestine. These carbohydrates can ferment in the gut, leading to the uncomfortable symptoms associated with IBS. By removing these trigger foods, the gut has a chance to calm down, and symptoms often subside.
The diet is implemented in three distinct phases: elimination, reintroduction, and personalization. The initial elimination phase, lasting 2-6 weeks, requires strict adherence to a low FODMAP food list. This phase aims to reduce symptoms by significantly limiting FODMAP intake. The following reintroduction phase involves systematically reintroducing specific FODMAP groups one at a time, while carefully monitoring symptoms. This process helps pinpoint which specific FODMAPs trigger your individual IBS symptoms. The final personalization phase focuses on creating a tailored long-term eating plan that minimizes trigger foods while maximizing nutritional variety.
The following infographic visually represents the three phases of the low FODMAP diet:
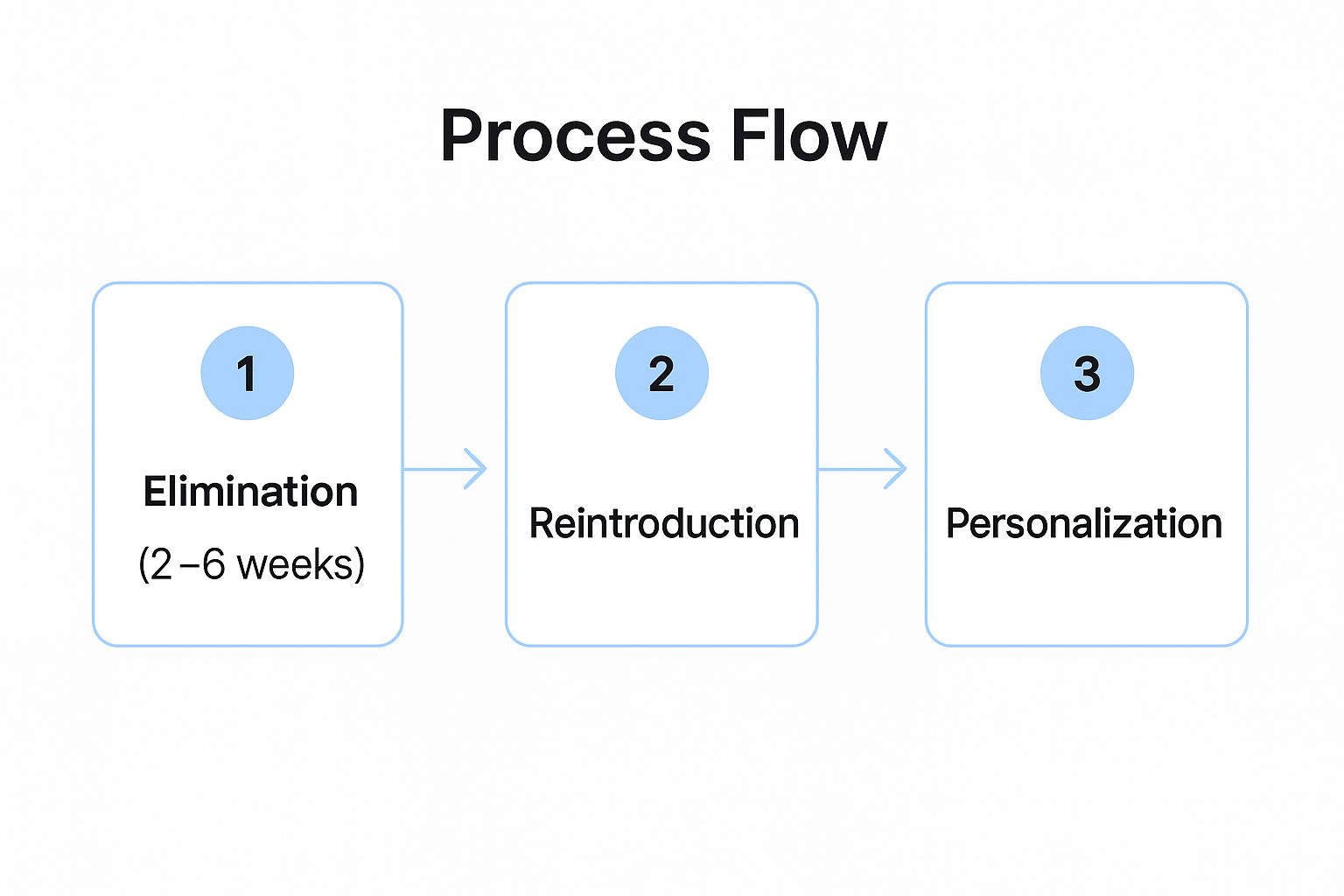
This step-by-step process illustrates the crucial flow from eliminating potential triggers to personalizing a long-term dietary strategy. The sequential nature of these phases is vital; skipping steps, particularly the reintroduction phase, can lead to unnecessarily restrictive eating habits.
This structured approach has proven remarkably effective, with studies like those conducted by Monash University, demonstrating a 68% symptom reduction in IBS sufferers following a low FODMAP diet. Learn more about Low FODMAP Diet. Success stories documented in gastroenterology journals further highlight its potential to dramatically improve quality of life for those living with IBS. On average, 70-80% of IBS patients experience significant symptom improvement using this method.
While highly effective, the low FODMAP diet does have potential drawbacks. The initial elimination phase can be quite restrictive, potentially making it nutritionally challenging without proper guidance. It's also a time-consuming process that requires meticulous planning and food tracking. Working with a registered dietitian experienced in FODMAPs is highly recommended to navigate these challenges and ensure nutritional adequacy.
Here are some essential tips for successfully implementing a low FODMAP diet:
- Work with a registered dietitian: A dietitian can provide personalized guidance, ensure nutritional balance, and help you navigate the complexities of the diet.
- Use the official Monash University FODMAP app: This app provides a comprehensive database of low and high FODMAP foods, making it easier to make informed food choices.
- Keep detailed food and symptom diaries: Tracking your food intake and symptoms is crucial for identifying your personal trigger foods.
- Don't skip the reintroduction phase: This phase is essential for identifying specific trigger foods and avoiding unnecessarily restrictive eating habits.
The low FODMAP diet, popularized by Monash University researchers, including Professor Peter Gibson and Dr. Sue Shepherd, along with prominent FODMAP dietitians like Kate Scarlata, offers a powerful tool for managing IBS pain. It empowers individuals to take control of their digestive health by understanding and managing their unique triggers. While it requires commitment and careful planning, the potential for significant and sustained relief from IBS pain makes the low FODMAP diet a worthwhile approach for many.
2. Peppermint Oil Capsules
For those seeking natural relief from the debilitating pain of Irritable Bowel Syndrome (IBS), peppermint oil capsules offer a promising solution. These capsules, specifically the enteric-coated variety, contain concentrated menthol, a natural compound known for its antispasmodic properties. This means it works directly on the smooth muscle of the intestinal tract, relaxing it to alleviate the cramping, bloating, and abdominal pain commonly associated with IBS. This makes peppermint oil a valuable tool in managing IBS pain and improving overall gut health. If you’re exploring options for what helps IBS pain, peppermint oil capsules are definitely worth considering.

Peppermint oil capsules typically contain 0.2-0.4ml of peppermint oil per capsule. The crucial element to look for is the enteric coating. This special coating protects the capsule as it passes through the stomach, preventing the peppermint oil from being released prematurely and causing potential heartburn or stomach upset. Instead, the coating allows the capsule to reach the small and large intestines, where the peppermint oil can be effectively released and act directly on the source of the discomfort. The mechanism of action involves blocking calcium channels in the smooth muscle, leading to muscle relaxation and pain relief. Peppermint oil capsules are readily available as an over-the-counter supplement, offering an accessible and natural approach to IBS symptom management.
The efficacy of peppermint oil for IBS is supported by clinical studies, some showing a remarkable 50% reduction in IBS symptoms. This makes it a compelling natural alternative to prescription medications, particularly for those seeking plant-based or vegan options for managing their gut health. Furthermore, when taken as directed, specifically with the enteric coating, peppermint oil capsules have relatively few side effects. This favorable safety profile, coupled with its fast-acting relief for acute symptoms, makes it a valuable tool for managing IBS flare-ups.
For instance, clinical trials published in the British Medical Journal (BMJ) have demonstrated significant pain reduction in IBS patients using peppermint oil. The use of peppermint oil as a first-line treatment for IBS is even prevalent in some European medical systems, further highlighting its recognized effectiveness. Positive outcomes have also been observed in pediatric IBS studies, suggesting its potential benefits across various age groups.
While peppermint oil capsules hold significant promise, it's important to be aware of potential drawbacks. As mentioned earlier, non-enteric coated capsules can induce heartburn. Peppermint oil may also interact with certain medications, so it's crucial to consult with a healthcare professional, especially if you're currently taking other medications. Additionally, peppermint oil is not suitable for individuals with gastroesophageal reflux (GERD) as it can worsen symptoms. Finally, the quality of peppermint oil capsules can vary significantly between brands, making it essential to choose reputable and pharmaceutical-grade products.
To maximize the benefits and minimize potential side effects, follow these tips:
- Choose enteric-coated capsules: This is paramount to prevent stomach irritation and ensure the oil reaches the intestines.
- Timing is key: Take the capsules 30-60 minutes before meals to allow them to work effectively.
- Start low and go slow: Begin with a lower dose to assess your tolerance and gradually increase if needed.
- Quality matters: Look for pharmaceutical-grade products to ensure purity and potency.
The popularity and acceptance of peppermint oil for IBS management have been driven by research and advocacy. Dr. Alex Ford, a researcher at the University of Leeds, has been instrumental in investigating the therapeutic effects of peppermint oil on IBS. Pharmaceutical brands like IBgard and FDgard have also played a significant role in bringing peppermint oil capsules to a wider audience. Furthermore, European gastroenterology associations have recognized the benefits of peppermint oil, contributing to its integration into clinical practice.
Peppermint oil capsules present a viable and natural option for individuals struggling with what helps IBS pain. Its ability to directly target intestinal smooth muscle, combined with its relatively safe profile and supporting clinical evidence, makes it a worthwhile addition to any IBS management strategy. However, remember to consult with a healthcare provider before starting any new supplement, especially if you have pre-existing conditions or are taking other medications. By making informed choices and following the recommended guidelines, you can harness the potential of peppermint oil to find much-needed relief from IBS pain and improve your overall quality of life.
3. Gut-Directed Hypnotherapy: A Mind-Body Approach to IBS Pain Relief
If you're searching for what helps IBS pain, gut-directed hypnotherapy might be a surprisingly effective option. This specialized form of clinical hypnotherapy isn't about swinging pocket watches. Instead, it uses the power of the mind-body connection to influence gut function and provide relief from the often debilitating symptoms of Irritable Bowel Syndrome (IBS). Unlike medications that simply mask symptoms, gut-directed hypnotherapy aims to address the underlying causes, offering a potentially long-term solution for managing IBS pain and discomfort.
Gut-directed hypnotherapy works by combining deep relaxation techniques with targeted suggestions specifically designed to impact the gastrointestinal system. The gut, often referred to as the "second brain," has its own complex nervous system that communicates directly with the brain. In individuals with IBS, this communication can become disrupted, leading to heightened sensitivity to pain, altered bowel motility, and increased stress perception. This therapy aims to re-establish healthy communication between the gut and the brain, restoring balance and reducing symptoms.
A typical gut-directed hypnotherapy program involves a structured protocol of 7-12 sessions. Each session combines deep relaxation exercises, such as progressive muscle relaxation and guided imagery, with gut-specific suggestions. These suggestions might focus on reducing gut sensitivity, normalizing bowel movements, and promoting a sense of calm and control over symptoms. Importantly, this therapy also addresses any underlying psychological factors, like stress and anxiety, that can contribute to IBS symptoms. The process empowers individuals to manage their condition more effectively and break the cycle of pain and stress.
The delivery method for gut-directed hypnotherapy can vary. It is often delivered in-person by a trained therapist, providing a personalized and supportive environment. However, for those with limited access to practitioners, validated audio programs can be a convenient and effective alternative. These programs, often developed by leading experts in the field, guide listeners through the same relaxation and suggestion techniques used in in-person sessions.
The effectiveness of gut-directed hypnotherapy for IBS has been demonstrated in several studies. Notably, research conducted at Manchester University by Professor Peter Whorwell, a pioneer in this field, has shown significant and long-lasting symptom improvement in approximately 71% of patients. These positive effects can often persist for years after treatment completion, offering sustained relief. Further solidifying its credibility, gut-directed hypnotherapy is implemented in specialized IBS clinics worldwide and its success has been documented in major gastroenterology journals. Examples include the work of Dr. Olafur Palsson at the University of North Carolina and the widespread use of programs like The IBS Audio Program by Michael Mahoney.
While gut-directed hypnotherapy offers considerable promise, it's important to be aware of both its advantages and disadvantages.
Pros:
- Significant symptom improvement in a majority of patients.
- Long-lasting effects, potentially lasting years after treatment.
- No side effects or drug interactions, making it a safe alternative or complement to medication.
- Holistic approach addressing both the physical and psychological aspects of IBS.
Cons:
- Limited availability of trained practitioners specializing in gut-directed protocols.
- Requires commitment to multiple sessions over several weeks.
- Often not covered by most insurance plans, which can make it financially challenging.
- Individual response varies, and it may not be effective for everyone.
Tips for maximizing the benefits of gut-directed hypnotherapy:
- Find a qualified practitioner: Seek out practitioners certified in gut-directed hypnotherapy protocols.
- Consider audio programs: If accessing a practitioner is difficult, explore validated audio programs like The IBS Audio Program.
- Practice regularly: Consistent practice between sessions is crucial for optimal results. This might involve listening to audio recordings or practicing self-hypnosis techniques.
- Integrate with other strategies: Combine gut-directed hypnotherapy with other IBS management strategies, such as dietary modifications, stress management techniques, and regular exercise, for a comprehensive approach to managing your symptoms.
If you're tired of searching for what helps IBS pain and are looking for a non-pharmacological approach that addresses the root causes of your symptoms, gut-directed hypnotherapy might be a valuable tool to explore. It offers a safe, effective, and potentially long-term solution for managing IBS and reclaiming control over your digestive health.
4. Probiotics (Specific Strains)
Irritable Bowel Syndrome (IBS) can significantly impact your quality of life, causing persistent abdominal pain, bloating, and altered bowel habits. While various approaches exist to manage IBS pain, modulating the gut microbiome through targeted probiotic supplementation has emerged as a promising strategy. If you're searching for what helps IBS pain, specific probiotic strains may offer much-needed relief. This approach focuses on introducing beneficial bacteria into your digestive system to address underlying imbalances that contribute to IBS symptoms.
The human gut is a complex ecosystem teeming with trillions of bacteria, collectively known as the gut microbiota. This intricate community plays a crucial role in digestion, immunity, and even mental well-being. In individuals with IBS, the composition and function of the gut microbiota are often disrupted, leading to inflammation, increased intestinal permeability (leaky gut), and altered bowel motility, all of which contribute to IBS pain. Probiotics aim to restore balance within this ecosystem.
Targeted probiotic supplementation doesn't involve just any probiotic; it requires using specific bacterial strains that have demonstrated efficacy in clinical trials for managing IBS symptoms. This is crucial because different strains have different mechanisms of action and target different aspects of gut health. For example, some strains are particularly effective at reducing inflammation, while others focus on improving gut motility or strengthening the intestinal barrier. Multi-strain formulations are often most effective, as they can address multiple IBS-related issues simultaneously. However, simply taking a multi-strain probiotic isn't enough; ensuring an adequate colony forming unit (CFU) count, typically 10 billion or higher, is essential for achieving therapeutic benefits.
Specific strains like Bifidobacterium infantis 35624 have shown remarkable promise in alleviating IBS symptoms. This particular strain has been extensively studied and is even FDA-approved for IBS. It works by reducing inflammation in the gut, improving gut motility, and normalizing bowel movements. Another example is the VSL#3 probiotic blend, which has demonstrated effectiveness in clinical trials for reducing bloating, abdominal pain, and improving overall IBS symptom severity. Multi-strain protocols are also increasingly being used in research settings to investigate the synergistic effects of various beneficial bacteria. These examples highlight the importance of selecting probiotics based on scientific evidence and clinical validation.
Learn more about Probiotics (Specific Strains)
While probiotics offer a promising avenue for managing IBS pain, it's essential to be aware of both their potential benefits and drawbacks.
Pros:
- Addresses underlying gut microbiome imbalances: Unlike medications that only mask symptoms, probiotics aim to address the root cause of IBS by restoring a healthy gut microbial balance.
- Generally safe with minimal side effects: Probiotics are generally well-tolerated, with side effects usually limited to mild and transient gas or bloating.
- May provide additional immune and digestive benefits: Beyond IBS relief, probiotics can contribute to overall digestive health and support a healthy immune system.
- Can be used long-term for maintenance: Once a positive response is achieved, probiotics can often be continued long-term to maintain gut health and prevent symptom recurrence.
Cons:
- Results vary significantly between individuals: The effectiveness of probiotics can vary depending on an individual's specific gut microbiota composition and the severity of their IBS.
- Quality and viability issues with many products: Not all probiotic supplements are created equal. Some products may contain lower CFU counts than advertised or may not properly protect the bacterial strains from degradation.
- Can initially worsen symptoms in some patients: Some individuals may experience a temporary increase in gas or bloating when they first start taking probiotics. This is usually temporary and resolves as the gut adjusts.
- Expensive for high-quality, effective formulations: High-quality probiotic supplements with clinically studied strains and guaranteed potency can be relatively expensive.
To maximize the benefits of probiotics for IBS pain, consider the following tips:
- Choose products with clinically studied strains: Look for probiotics that contain strains specifically shown to be effective for IBS, such as B. infantis 35624 or the strains found in VSL#3.
- Start with lower doses to assess tolerance: Gradually increase the dosage as tolerated to minimize potential side effects.
- Look for third-party tested products with guaranteed potency: This ensures that the product contains the stated number of live bacteria and is free from contaminants.
- Take consistently for at least 4-8 weeks to assess effectiveness: It takes time for probiotics to colonize the gut and exert their beneficial effects. Be patient and consistent with your intake.
Research by prominent gastroenterologists like Dr. Eamonn Quigley and endorsements from organizations like the International Probiotic Association further support the potential of probiotics for IBS management. While probiotics are not a magic bullet, they can be a valuable tool in your arsenal for what helps IBS pain and improving overall gut health. They offer a natural, relatively safe, and potentially long-term solution for managing this chronic condition.
5. Stress Management and Mindfulness
Stress is a common trigger for IBS symptoms. For many, psychological stress can exacerbate existing symptoms or even initiate a flare-up. This connection highlights the powerful influence of the gut-brain axis, the bidirectional communication pathway between the central nervous system and the enteric nervous system (the "brain" in your gut). This intricate relationship means that emotional and psychological states can directly impact your digestive health, making stress management a vital component of managing IBS pain and discomfort. If you're exploring what helps IBS pain, addressing stress through mindfulness is a powerful tool you shouldn't overlook.
Stress management, particularly through mindfulness techniques, offers a targeted approach to calming this gut-brain axis dysfunction. Mindfulness practices encourage a focused awareness on the present moment without judgment, helping to reduce the impact of stress on both the mind and body. This approach includes various evidence-based techniques such as mindfulness meditation, deep breathing exercises, and progressive muscle relaxation. Each of these practices works synergistically to interrupt the cycle of stress-induced IBS symptoms.
Mindfulness meditation involves focusing on your breath, bodily sensations, thoughts, and emotions as they arise without getting carried away by them. This practice cultivates a sense of calm and allows you to observe your stress response rather than becoming overwhelmed by it. Deep breathing exercises help regulate the autonomic nervous system, promoting relaxation and reducing the physical manifestations of stress, such as muscle tension and rapid heart rate, which can indirectly alleviate IBS symptoms. Progressive muscle relaxation involves systematically tensing and releasing different muscle groups in the body, promoting physical relaxation and reducing overall stress levels.
The benefits of incorporating these stress management techniques are multifaceted. Firstly, they address a root cause of stress-induced IBS symptoms by directly targeting the gut-brain axis. This approach not only helps manage current symptoms but can also prevent future flare-ups. Additionally, these practices offer broader mental health benefits, reducing anxiety, improving sleep quality, and enhancing overall well-being. A significant advantage is that mindfulness techniques are often free when self-directed, requiring no special equipment or costly memberships. They also complement other IBS treatments effectively, working in tandem with dietary modifications, medications, and other therapies.
For those new to mindfulness, even short bursts of practice can be beneficial. Practicing mindfulness can significantly reduce stress and improve IBS symptoms. Try these quick mindfulness exercises to calm your mind. Starting with just 10-15 minutes of daily practice can make a noticeable difference. Guided meditation apps designed specifically for IBS can provide structured support and personalized practices. Incorporating belly breathing during symptom flares can offer immediate relief by calming the nervous system and reducing muscle tension in the abdomen. For more in-depth support, consider professional stress management counseling, especially if stress significantly impacts your daily life and IBS symptoms.
Examples of successful implementations of stress management for IBS include Mindfulness-Based Stress Reduction (MBSR) programs, pioneered by Dr. Jon Kabat-Zinn. These programs offer structured training in mindfulness meditation and have shown significant positive results in reducing IBS symptoms. Hospital-based IBS stress management programs, often led by experts like Dr. Brenda Toner, a prominent researcher in IBS-focused mindfulness, provide comprehensive and tailored support for individuals struggling with the condition. Increasingly, gastroenterology practices are integrating stress management protocols into their treatment plans, recognizing the importance of addressing the gut-brain connection. Popular apps like Headspace and Calm also offer readily available resources for guided meditations and mindfulness exercises.
While stress management and mindfulness offer significant potential for IBS relief, it's important to acknowledge that these techniques require consistent practice to be effective. The benefits may take weeks or even months to become fully apparent, requiring patience and commitment. Some techniques, particularly progressive muscle relaxation, may benefit from initial professional guidance to ensure proper form and maximize effectiveness. It's also crucial to understand that individual responses to these practices vary considerably. What works well for one person may not be as effective for another. Finding the right approach often involves experimentation and adapting the techniques to suit your individual needs and preferences. Despite these potential challenges, the long-term benefits of incorporating stress management and mindfulness into your IBS management plan can be substantial, leading to improved symptom control, enhanced well-being, and a greater sense of control over your health.
6. Soluble Fiber Supplementation
Irritable Bowel Syndrome (IBS) can significantly impact daily life, with abdominal pain being a hallmark symptom. If you're searching for what helps IBS pain, soluble fiber supplementation deserves serious consideration. Unlike insoluble fiber, which adds bulk to stool and can exacerbate certain IBS symptoms, soluble fiber dissolves in water to form a gel-like substance. This gel has unique properties that can regulate bowel movements, reduce discomfort, and foster a healthier gut environment. For many battling IBS, strategic use of soluble fiber supplements, particularly psyllium husk, has emerged as a key component of effective symptom management.
So how does soluble fiber work its magic? It primarily acts by normalizing intestinal transit time. For those with IBS-C (constipation-predominant), the gel adds bulk and moisture to the stool, easing its passage through the digestive tract and alleviating painful constipation. Conversely, in individuals with IBS-D (diarrhea-predominant), the same gel can help absorb excess water, adding form to loose stools and reducing the frequency and urgency of bowel movements. Beyond regulating transit time, soluble fiber acts as a prebiotic, providing nourishment for beneficial bacteria in the gut. This promotes a balanced gut microbiome, crucial for overall digestive health and reducing inflammation which often contributes to IBS pain.
Psyllium husk is the most clinically supported form of soluble fiber for IBS. Its efficacy has been demonstrated in multiple randomized controlled trials showing significant improvement in abdominal pain, bloating, and stool consistency. Companies like Metamucil have also conducted extensive clinical studies in IBS populations further solidifying psyllium's place in IBS management. In fact, its benefits are so well-established that psyllium husk is integrated into IBS treatment guidelines worldwide, including those published by the American College of Gastroenterology. You can learn more about Soluble Fiber Supplementation.
The advantages of psyllium husk extend beyond its effectiveness. It’s a natural, plant-based option generally well-tolerated by most patients, fitting seamlessly into vegan and plant-based lifestyles. Furthermore, it's relatively inexpensive and readily available in most pharmacies and health food stores. Interestingly, research suggests psyllium husk may also offer additional cardiovascular and metabolic benefits, making it a valuable addition to any health-conscious individual's routine, not just those struggling with IBS.
While generally safe, psyllium husk supplementation does come with a few caveats. It's crucial to significantly increase water intake when using this supplement. The fiber absorbs water to form its beneficial gel, and inadequate fluid intake can lead to dehydration or even worsen constipation. Initially, some individuals may experience bloating and gas, particularly if they introduce the supplement too quickly. Starting with small doses and gradually increasing is essential to minimize these side effects. Finally, psyllium husk can interfere with the absorption of certain medications. It's advisable to time your psyllium husk intake at least two hours away from other medications to avoid potential interactions.
To maximize the benefits and minimize potential downsides, consider the following tips:
- Start Low and Go Slow: Begin with a very small dose, such as 1/4 teaspoon of psyllium husk, and gradually increase the amount over several weeks as your body adjusts.
- Hydrate, Hydrate, Hydrate: Drink plenty of water with each dose of psyllium husk, aiming for at least 8 ounces per serving. Maintaining adequate hydration throughout the day is also essential.
- Time it Right: Separate your psyllium husk intake from other medications by at least two hours to prevent interference with absorption.
- Choose Wisely: Opt for pure psyllium husk without artificial additives, flavors, or sweeteners.
For individuals seeking relief from IBS pain, exploring what helps IBS pain often leads to soluble fiber. Psyllium husk, in particular, stands out for its proven effectiveness in managing both IBS-C and IBS-D symptoms, its natural origin, and its affordability. By following the guidelines and tips outlined above, you can safely and effectively incorporate psyllium husk into your routine, potentially experiencing significant improvement in your IBS symptoms and overall gut health. Remember to consult with your healthcare provider or a registered dietitian before starting any new supplement regimen, especially if you have underlying health conditions or are taking other medications. They can help you determine the appropriate dosage and ensure it aligns with your individual health needs.
7. Heat Therapy and Abdominal Massage
Dealing with the cramping, bloating, and general discomfort of IBS can be debilitating. When searching for "what helps ibs pain," many find relief through drug-free, accessible methods like heat therapy and abdominal massage. These physical comfort measures offer immediate, targeted relief by relaxing tense intestinal muscles, improving blood flow to the gut, and reducing pain perception during IBS flares. This combination approach addresses both the physical and neurological aspects of IBS pain, making it a valuable tool for managing symptoms.

Heat therapy works by increasing blood circulation to the applied area. This increased blood flow delivers oxygen and nutrients while flushing away metabolic waste products that can contribute to pain and inflammation. The warmth also has a direct soothing effect on the intestinal muscles, helping to relax spasms and ease cramping. Abdominal massage further enhances these benefits by physically manipulating the tissues and stimulating the digestive tract. Gentle, clockwise circular motions, following the path of the colon, can help to relieve trapped gas, promote bowel movements, and further reduce muscle tension. The combined effect of heat and massage creates a synergistic approach to pain management, tackling the discomfort from multiple angles.
The beauty of this method lies in its accessibility and safety. Unlike medications, heat therapy and abdominal massage are drug-free and carry minimal risk of side effects for most individuals. They can be easily self-administered at home, making them a convenient and cost-effective option for managing IBS pain whenever it strikes. This makes it particularly appealing for those seeking natural and holistic approaches to gut health, including those following plant-based or vegan lifestyles.
Here are some examples of how this combined therapy has been successfully implemented:
- Hospital Pain Management: Heat therapy is frequently incorporated into hospital pain management protocols for various conditions, including IBS, demonstrating its efficacy in clinical settings.
- Physical Therapy Integration: Increasingly, physical therapists are integrating abdominal massage techniques into IBS treatment plans, recognizing the importance of addressing the musculoskeletal component of this condition.
- IBS Support Groups: Many IBS self-help and support groups teach self-care programs that incorporate heat therapy and abdominal massage as core components for at-home pain management.
To maximize the benefits of heat therapy and abdominal massage for IBS pain, consider these practical tips:
- Apply Heat Wisely: Use a heating pad set on low to medium heat for 15-20 minutes at a time. Avoid high heat settings, which can burn the skin.
- Master the Massage: Practice gentle, clockwise circular massage motions following the natural path of the colon. This video provides a visual guide to effective abdominal massage techniques:
- Breathe Deeply: Combine heat therapy and massage with deep breathing exercises to enhance relaxation and further reduce stress, a known IBS trigger.
- Be Prepared On-the-Go: Keep portable heat packs readily available for use away from home, empowering you to manage IBS pain in various settings.
While heat therapy and abdominal massage offer significant benefits for IBS pain relief, it’s important to acknowledge some limitations. The effects are typically temporary and primarily address symptoms rather than the underlying causes of IBS. Implementing these techniques also requires dedicated time and a degree of privacy, which might not always be feasible. Furthermore, while basic massage techniques are easy to learn, more advanced methods may require guidance from a healthcare professional or physical therapist.
Despite these limitations, the immediate, drug-free relief, accessibility, and ease of use make heat therapy and abdominal massage a valuable addition to any IBS management strategy. This combined approach, championed by organizations like the International Association of Healthcare Practitioners, IBS self-help organizations, and physical therapy associations, empowers individuals to take control of their IBS pain and improve their quality of life.
8. Antispasmodic Medications
Dealing with the unpredictable pain of Irritable Bowel Syndrome (IBS) can be incredibly disruptive. If you're searching for what helps IBS pain, antispasmodic medications are a valuable tool to consider, offering targeted relief from the cramping and discomfort that often accompany this condition. These medications work directly on the smooth muscles of your intestines, calming the spasms that are a major source of IBS pain. This makes them a practical choice for managing acute episodes and improving overall quality of life.
Antispasmodics work by relaxing the smooth muscles in the gastrointestinal tract. In IBS, these muscles can contract erratically and forcefully, leading to the characteristic cramping pain. These medications interfere with the signaling pathways that trigger these contractions, effectively reducing their intensity and frequency. This targeted action makes them particularly effective for managing IBS symptoms dominated by cramping and spastic pain.
Several different classes of antispasmodics exist, providing options for both prescription and over-the-counter relief. Hyoscine butylbromide (known as scopolamine butylbromide in some regions), mebeverine, and dicyclomine are among the most commonly prescribed. These medications are available in various forms, including tablets, capsules, and liquid solutions, allowing for flexibility in administration. The availability of both prescription and over-the-counter options allows for tailored treatment plans based on individual needs and symptom severity. For instance, milder, occasional symptoms might be managed with an over-the-counter antispasmodic, while more persistent or severe pain may require a prescription-strength medication.
One of the key advantages of antispasmodics is their rapid onset of action. For those experiencing a sudden bout of IBS pain, these medications can provide relatively quick relief, often within minutes to an hour. This fast-acting nature makes them a valuable tool for managing acute episodes and preventing them from disrupting daily activities. Furthermore, they can be used either as needed for immediate relief or on a regular basis to prevent symptoms. The dosage can also be adjusted ("titrated") according to individual needs and responses, allowing for personalized treatment strategies.
Several studies and clinical trials have demonstrated the effectiveness of antispasmodics for IBS pain relief. For example, Buscopan (hyoscine butylbromide), widely used in Europe and other parts of the world, has shown superior efficacy compared to placebo in reducing abdominal pain and improving bowel function in IBS patients. Similarly, Bentyl (dicyclomine), commonly prescribed in North America, has a long history of use and has been proven effective in relieving IBS-related cramping. These clinical trials, often backed by gastroenterology medical associations and pharmaceutical companies like Boehringer Ingelheim, contribute to the inclusion of antispasmodics in global IBS treatment guidelines.
While antispasmodics offer significant benefits for managing IBS pain, it's important to be aware of potential drawbacks. Some common side effects include dry mouth, blurred vision, and drowsiness. These side effects are usually mild and transient, but they can be bothersome for some individuals. Additionally, antispasmodics don’t address the underlying causes of IBS. They treat the symptoms, not the root of the problem. This means that they are typically used as part of a comprehensive management plan that may also include dietary modifications, stress management techniques, and other lifestyle changes. Some individuals may also develop a tolerance to these medications over time, requiring dosage adjustments or a switch to a different medication. Finally, interactions with other medications are possible, so it’s crucial to discuss your medication history with your healthcare provider before starting antispasmodics.
Here are some practical tips for using antispasmodics effectively:
- Take at the first sign of cramping: For the best results, take the medication as soon as you feel cramping beginning. This can help prevent the pain from escalating.
- Start with the lowest effective dose: Begin with the lowest recommended dose and only increase it if necessary. This can minimize the risk of side effects.
- Be mindful of potential drowsiness: If you experience drowsiness, avoid driving or operating machinery.
- Discuss with your healthcare provider: Always consult with your doctor or another qualified healthcare professional before starting any new medication, especially if you are taking other medications or have any underlying health conditions. They can help you determine the appropriate medication and dosage for your individual needs.
Antispasmodic medications provide a valuable option for those seeking what helps IBS pain. Their targeted action, rapid onset, and availability in both prescription and over-the-counter forms make them a useful tool in managing the challenging symptoms of IBS. However, understanding both the benefits and potential side effects is essential for informed decision-making and effective symptom control. Remember to always consult with your healthcare provider before starting any new medication.
8 IBS Pain Relief Strategies Compared
| Remedy / Strategy | Implementation Complexity 🔄 | Resource Requirements 💡 | Expected Outcomes 📊 | Ideal Use Cases 💡 | Key Advantages ⭐⚡ |
|---|---|---|---|---|---|
| Low FODMAP Diet | Moderate to High: 3 phases over 2-6 weeks | Dietitian support often needed; planning | 70-80% symptom improvement | IBS patients needing trigger identification | Long-term management; evidence-backed ⭐ |
| Peppermint Oil Capsules | Low: Simple oral supplement, OTC availability | Low cost; need to select quality capsules | ~50% symptom reduction | Acute relief of cramping and bloating | Fast-acting; natural alternative ⚡ |
| Gut-Directed Hypnotherapy | High: 7-12 sessions, requires trained practitioner | Access to certified therapists or programs | 71% patients achieve significant relief | IBS with psychological or gut-brain aspects | Long-lasting effects; no side effects ⭐ |
| Probiotics (Specific Strains) | Low to Moderate: daily supplementation | Purchase of high-quality strains | Variable; can improve gut balance | Long-term symptom modulation | Addresses microbiome; safe for most |
| Stress Management & Mindfulness | Moderate: daily practice, potential professional guidance | Minimal cost if self-guided; apps available | Gradual symptom improvement | Stress-related IBS symptom triggers | Mental health benefits; no side effects ⭐ |
| Soluble Fiber Supplementation | Low: Oral powder or capsules, gradual introduction | Inexpensive; requires water intake | Improvement in bowel regularity | IBS with constipation or diarrhea | Natural, multi-symptom relief |
| Heat Therapy & Abdominal Massage | Low: Self-administered, needs proper technique | Minimal (heat pack, time) | Temporary symptom relief | Acute pain and cramping episodes | Rapid relief; no side effects ⚡ |
| Antispasmodic Medications | Low to Moderate: as needed dosing | Prescription or OTC purchase | Rapid cramp and pain reduction | Acute IBS cramping and spastic pain | Fast symptom relief; titratable doses |
Finding Your IBS Pain Relief Toolkit
Living with IBS pain can be challenging, but finding effective relief is within your reach. This article explored eight potential solutions for what helps IBS pain, from dietary changes like the low FODMAP diet and soluble fiber supplementation to targeted therapies such as peppermint oil capsules, specific probiotic strains, gut-directed hypnotherapy, and antispasmodic medications. We also touched on the importance of stress management and mindfulness, as well as the soothing benefits of heat therapy and abdominal massage.
Mastering these approaches isn't just about reducing pain; it's about reclaiming your life. By experimenting with and incorporating these strategies, you can create a personalized toolkit to manage your IBS symptoms and improve your overall well-being, from enjoying meals without worry to participating in activities you love. Remember, what helps IBS pain varies from person to person. Consulting with a healthcare provider is crucial to tailor a plan specific to your needs and medical history.
Taking control of your gut health starts with making informed choices. For convenient and effective hydration support, especially important when managing IBS, explore Cantein’s innovative hydration solutions. Staying properly hydrated can play a vital role in easing IBS symptoms and supporting overall digestive health. Learn more about how Cantein can complement your IBS management plan by visiting Cantein.

